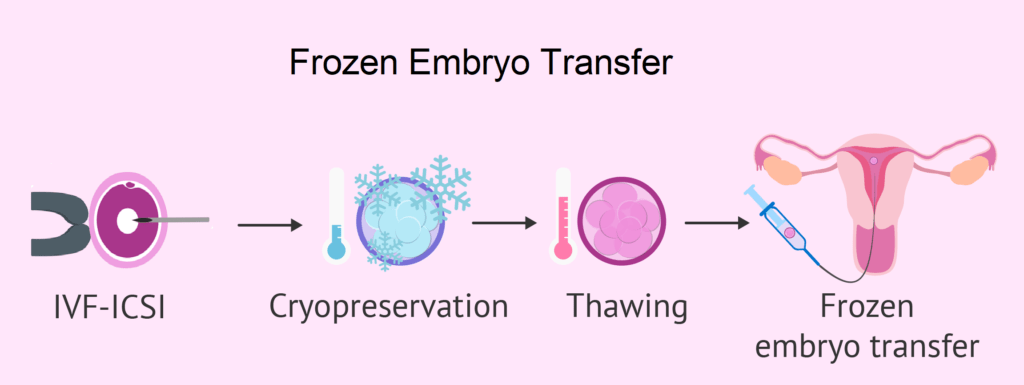
This is the name given to the process in which the embryos formed and frozen in an IVF cycle, are replaced in the uterus in a subsequent month.
Patient is seen on day 1 or 2 of periods.
We do a transvaginal scan to confirm the absence of any cysts.
Medication may be started in case of a hormonal cycle
Ultrasound monitoring of the endometrial lining is done starting about day 10 of cycle
Once the lining reaches a satisfactory thickness, progesterone is started.
Embryo transfer is planned after 3-5 days of progesterone depending on whether day 3 or day 5 embryos need to be replaced.
Embryo transfer is done under ultrasound guidance.
Luteal phase support with injections or medicines is advised for two weeks.
Beta hCG blood test is taken after 12 -14 days of transfer.
We usually expect a minimum of 8 mm thickness before replacing the embryos.
The lining may be unsatisfactory in one month and pick up in other months or with different methods of endometrial preparation as discussed before. In few women with persistently thin endometrium, we may have to rule out few causes like;
The endometrial lining in an ongoing IVF cycle may be suboptimal due to a state of increased oestrogen production and hence where there are multiple follicles developing, we prefer to freeze all the embryos and replace them at a later date.
Also, in such patients, we have the very important advantage of avoiding OHSS when we give an agonist trigger, freeze all and plan FET at a later date.
When the endometrial lining is more than 14-15 mm, the pregnancy rates may decrease and hence it is better to postpone transfer and rule out any pathology in the uterus like
A minimum of 8 days of oestrogen intake is advisable for adequate endometrial preparation. Though maximum duration has been reported upto even 40-60 days, usually we give for a period of 15-25 days before deciding to transfer or cancel the cycle.