Hysteroscopy is a procedure used to examine the inside of the uterus. A hysteroscopy usually takes between 5 and 30 minutes.
Procedure:
An instrument called a speculum may be inserted into the vagina to hold it open, although this is not always needed. The vagina and cervix are cleaned with an antiseptic solution. A hysteroscope (long, thin tube containing a light and camera) is passed into the uteus – you may experience some cramping and discomfort as it passes through your cervix.
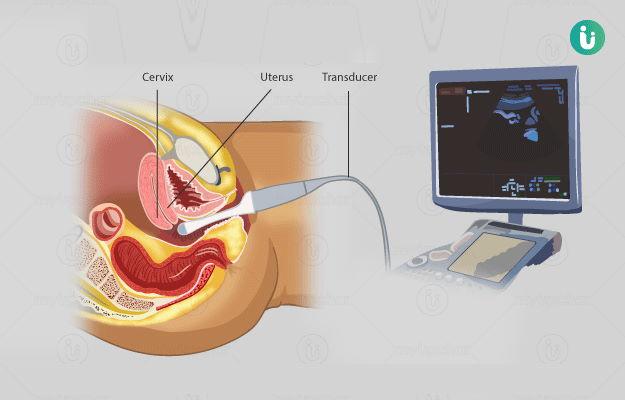
Fluid such as saline or glycine is gently pumped into the uterus to make it easier for the doctor to see inside. The camera sends pictures to a monitor so the doctor can spot any abnormalities if present.
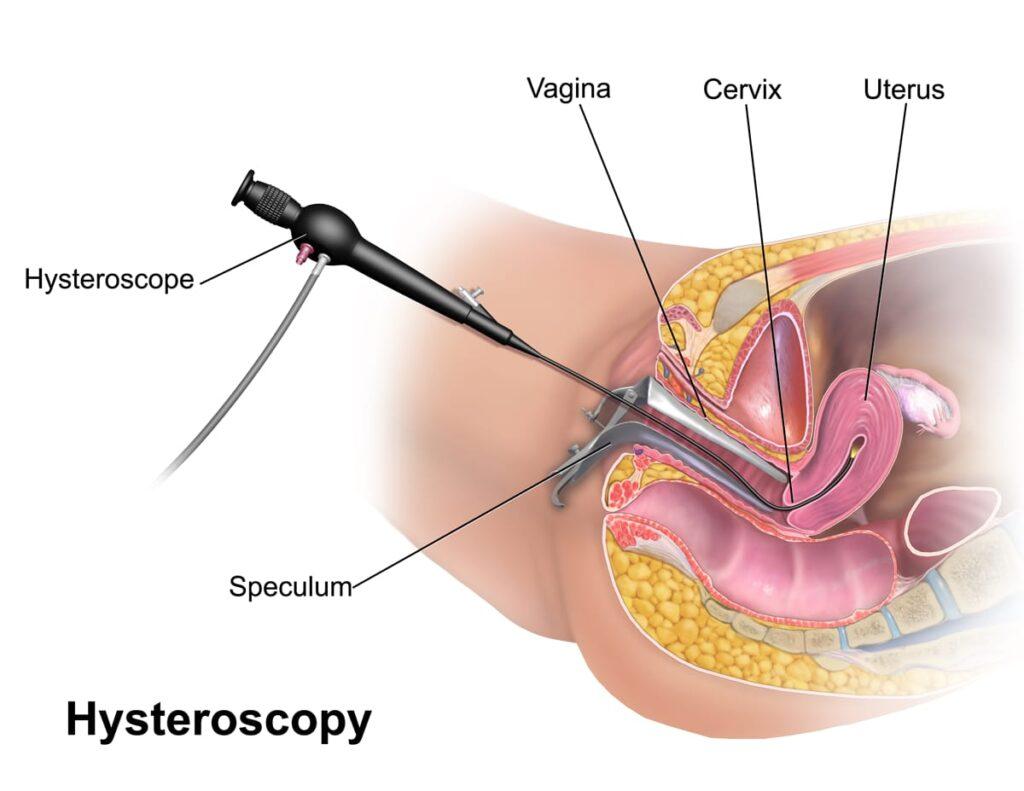
Hysteroscopy is a minimally invasive procedure used to examine the inside of the uterus using a thin, lighted instrument called a hysteroscope. It helps doctors diagnose and treat uterine abnormalities such as polyps, fibroids, adhesions, or structural issues that may affect fertility or implantation.
When couples experience difficulty conceiving, evaluating the health of the uterus becomes an important step in fertility assessment. One procedure frequently recommended for this purpose is hysteroscopy.
Hysteroscopy allows fertility specialists to directly view the uterine cavity and identify conditions that may interfere with pregnancy. Unlike imaging tests alone, this procedure provides a detailed examination and can sometimes treat certain uterine abnormalities during the same procedure.
Understanding how hysteroscopy works and why it is performed can help patients feel more confident when undergoing fertility evaluation.
Hysteroscopy is a diagnostic or surgical procedure used to examine the inside of the uterus.
During hysteroscopy:
This allows specialists to detect abnormalities affecting fertility or menstrual health.
Doctors recommend hysteroscopy to diagnose or treat conditions inside the uterus that may affect fertility.
Common reasons include:
Hysteroscopy provides more precise information than imaging tests alone.
Hysteroscopy may be recommended when:
The procedure is often performed after tests such as HSG or SSG identify possible concerns.
Used to examine the uterus and identify abnormalities affecting fertility or menstrual health.
Used to treat conditions found during examination, such as:
Operative hysteroscopy can sometimes improve fertility outcomes.
The procedure is usually scheduled after menstruation when the uterine lining is thin and easier to examine.
Patients may be advised to:
During hysteroscopy:
The procedure usually takes 10–30 minutes, depending on whether it is diagnostic or operative.
Hysteroscopy can identify several uterine conditions affecting fertility, including:
These conditions may interfere with implantation or pregnancy.
Most diagnostic hysteroscopy procedures cause only mild discomfort similar to menstrual cramps. Some procedures are performed under local or general anesthesia depending on complexity.
Doctors recommend appropriate pain management to ensure patient comfort.
Hysteroscopy is generally considered a safe procedure. Complications are uncommon but may include:
Your doctor will explain potential risks and safety precautions before the procedure.
Different tests evaluate different aspects of fertility.
Test | Purpose |
HSG | Detect tubal blockage |
SSG | Evaluate tubes and uterus |
Hysteroscopy | Directly examine uterine cavity |
Laparoscopy | Evaluate pelvic organs and endometriosis |
Doctors may combine these tests to get a complete fertility diagnosis.
In some cases, hysteroscopy can improve fertility when it removes abnormalities such as:
Treating these conditions may help improve implantation and pregnancy outcomes.
However, results vary depending on individual medical conditions.
In some cases, a small sample of tissue from the uterus lining may be removed for further testing. This is known as an endometrial biopsy.
If the findings of hysteroscopy needs to be treated such as fibroids or polyps, fine surgical instruments can be passed along the hysteroscope. These are used to cut or burn away the abnormal tissue.
Indications for a hysteroscopy:
Types of hysteroscopy:
Office hysteroscopy – done without anaesthesia in the OPD
Diagnostic Hysteroscopy – done under anaesthesia or mild sedation in the operation theatre
Operative hysteroscopy- done under anaesthesia and involves some operative procedure like removal of polyps or fibroids.
Hysteroscopy is considered minor surgery and usually does not require an overnight stay in the hospital.
If the cervix needs to be dilated, a local anesthesia is injected into the cervix since the dilation can otherwise be relatively painful. The average pain score during office hysteroscopy is 2 to 3 on a scale from zero to 10, where zero is no pain and 10 is worst pain.
Most women feel they can return to normal activities, including work, the day after having a hysteroscopy. Some women return to work later the same day. However, you may wish to have a few days off to rest, particularly if you had treatment such as fibroid removal and/or a general anaesthetic was used.
It is normal to have some mild cramping or a little bloody discharge for a few days after the procedure. You may be given medication to help ease the pain. If you have a fever, chills, or heavy bleeding, call your doctor right away.
Not always, but it may be recommended if imaging tests suggest uterine abnormalities.
Most patients recover quickly and resume normal activities within a day.
Yes, it can identify structural issues that may affect implantation.
Diagnostic hysteroscopy is minimally invasive, while operative hysteroscopy may involve minor surgical treatment.